Total hip arthroplasty is a surgical procedure that treats end-stage hip osteoarthritis and other debilitating hip conditions. However, postoperative pain remains a significant concern, as inadequate analgesia can delay mobilization, prolong hospital stays, and increase complication risks. Regional anesthesia techniques have evolved to address these challenges, and, among them, the pericapsular nerve group (PENG) block has gained attention. Recently, modified pericapsular nerve blocks have emerged as refinements aimed at improving analgesic efficacy while preserving motor function in total hip arthroplasty.
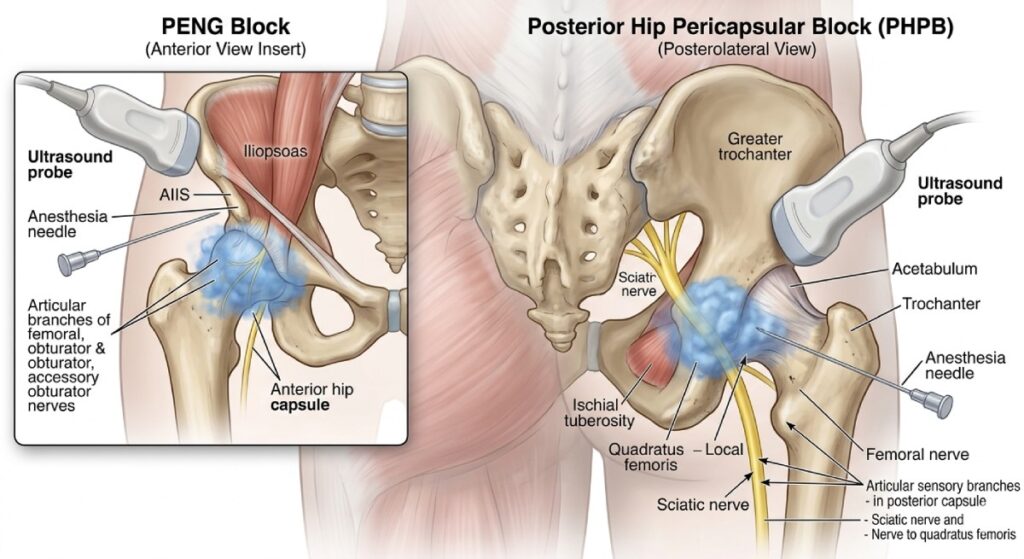
Effective pain control following total hips requires targeting the sensory innervation of the anterior hip capsule, which is primarily supplied by branches of the femoral, obturator, and accessory obturator nerves. Traditional blocks such as the femoral nerve block or fascia iliaca block often provide incomplete analgesia and may cause quadriceps weakness. The original PENG block was designed to selectively anesthetize articular branches supplying the anterior capsule while minimizing motor involvement. Modified approaches build on this concept by adjusting injection sites, volumes, or combining blocks to improve coverage of the hip joint’s complex innervation 1.
The development of modified pericapsular nerve blocks stems from the need to balance effective analgesia with early mobilization in total hip arthroplasty patients. In fast-track arthroplasty protocols, preserving motor strength is critical for early ambulation and reduced fall risk. Modifications may include altering needle trajectory under ultrasound guidance, expanding local anesthetic spread toward the iliopsoas plane, or combining the PENG block with lateral femoral cutaneous or obturator nerve blocks. These refinements aim to address posterior capsule pain and cutaneous components often missed by the original technique 2,3.
In clinical practice, modified pericapsular blocks are increasingly incorporated into multimodal analgesia pathways for this procedure. Studies suggest that patients receiving these blocks report lower postoperative pain scores, reduced opioid consumption, and improved satisfaction. Importantly, many modified approaches demonstrate minimal impact on quadriceps strength, enabling earlier participation in physiotherapy. This aligns well with enhanced recovery following surgery (ERAS) protocols, where early mobilization is a cornerstone of improved outcomes 2,4,5.
Despite promising results, modified pericapsular nerve blocks are not without limitations. Evidence is still evolving, with variations in technique, local anesthetic volumes, and outcome measures across studies. Operator expertise in ultrasound-guided regional anesthesia is crucial, as improper placement can reduce effectiveness. Furthermore, while motor-sparing is a major advantage, inconsistent blockade of obturator or posterior capsule innervation might still result in residual pain in some patients 5,6.
Ongoing research aims to standardize modified techniques and define optimal dosing strategies. Comparative trials evaluating different modifications, combinations with other regional blocks, and long-term functional outcomes are needed. Advances in imaging and injection technology may further improve accuracy and reproducibility. As evidence grows, modified pericapsular nerve blocks have the potential to become a central component of personalized analgesia strategies for total hip arthrooplasty.
References
1. NYSORA. The Hip (PENG) Block. NYSORA https://www.nysora.com/education-news/the-hip-block-new-addition-to-nysoras-web-app/ (2020).
2. Hu, J., Wang, Q., Hu, J., Gong, C. & Yang, J. A modified hip pericapsular nerve block on postoperative pain and functional outcome after total hip arthroplasty: a prospective, double-blind, randomized controlled study. Korean J Anesthesiol 78, 351–360 (2025). DOI: 10.4097/kja.24593
3. Ben Aziz, M. & Mukhdomi, J. Pericapsular Nerve Group Block. in StatPearls (StatPearls Publishing, Treasure Island (FL), 2025).
4. Yu, L., Shen, X. & Liu, H. The efficacy of pericapsular nerve group block for postoperative analgesia in patients undergoing hip surgery: A systematic review and meta-analysis of randomized controlled trials. Front. Med. 10, (2023). DOI: 10.3389/fmed.2023.1084532
5. Tian, Y. et al. The effect of pericapsular nerve group block and lateral femoral cutaneous nerve block on postoperative recovery after hip arthroplasty. Sci Rep 15, 19913 (2025). DOI: 10.1038/s41598-025-04699-6
6. Buono, R. D., Pascarella, G., Costa, F., Terranova, G. & Tognù, A. Hip arthroplasty under pericapsular nerve group blocks combined with local anesthesia. Advances in Anesthesia and Pain Medicine 3, (2025). DOI: 10.4081/aapm.2025.45